By: Dr. Anna Kuljian, PT, DPT
The Cliff Notes:
If you have shoulder pain, you’re not alone because 7-34% of adults have shoulder pain! Let’s zoom in on a shoulder that is painful and weak, which commonly includes subacromial pain syndrome (SAPS) and rotator cuff related shoulder pain. It usually involves non-traumatic one-sided pain on the front and outer parts of the shoulder that feels worse when lifting the arm, especially in the middle range, laying on it, and holding a thumbs down position against resistance. While imaging is usually not necessary, diagnosis is typically based on symptoms, past medical history, and clinical examination. It can last anywhere from 6-18 months depending on how long you’ve had it. And PT can help!
Who Gets It?
Affected patients are most often in their 50s and the number of people/year increases with age. Subacromial pain is considered to be one of the most common musculoskeletal conditions affecting the shoulder. In fact, 89% of all shoulder complaints referred to PTs and general practitioners are subacromial.
What Causes It?
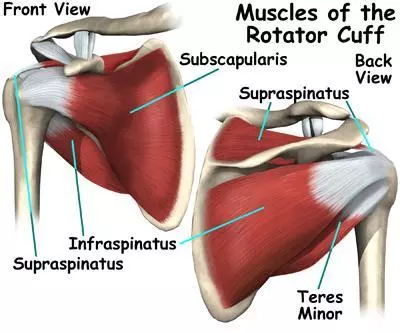
The rotator cuff consists of four muscles that support the shoulder girdle, shown above. Subacromial pain syndrome may be caused by rotator cuff tendons that degenerate internally and may eventually develop into tears. Imaging research studies demonstrated a large percent of individuals who did not have symptoms but had evidence of structural failure like a full thickness rotator cuff tear. So, there is no clinical certainty that those abnormalities seen in imaging are the actual cause of symptoms. Hypotheses that the acromion bone irritates or impinges the soft tissues under it, the bursa and rotator cuff have not been proven. Overall, muscle weakness, tightness, posture, and alignment may contribute to shoulder pain.
How Is It Treated?
⦁ The overall goals of PT are to reduce pain and improve function with daily activities, mobility, strength, and quality of life.
⦁ Therapeutic exercises address weakness, tightness, posture, and alignment in and around the shoulder girdle, neck, and thoracic/mid spine.
⦁ Therapeutic activities are functional activities such as lifting or carrying a bag of groceries, pushing open a heavy door, and reaching for items out of a high cabinet. If you have pain while sleeping, positioning and pillow placement will be discussed.
⦁ Manual therapy includes massaging tight or guarded muscles, assisted stretches, muscle activation re-education like “PNF”, trigger point release, and joint mobilizations to the shoulder girdle, neck, or thoracic/mid spine.
⦁ Modalities include ice or heat, cold laser therapy, and taping techniques.
⦁ SAPS is preferably treated non-operatively.
⦁ There is strong evidence showing that supervised non-operative rehabilitation diminishes shoulder pain and improves function.
⦁ Conservative treatment should be considered for up to about 1 year until there is improvement and returned function.
⦁ For recurrent or persistent symptoms, corticosteroid injection is indicated.
⦁ Surgery should only be considered after carrying out a structured rehabilitation program for the appropriate amount of time and if not responding to exhaustive non-surgical treatments. However, there is no convincing evidence that surgery is more effective than conservative management for SAPS.
What Can You Do About It?
Some tips are to avoid reaching above shoulder height or behind your back. Gentle exercises and stretching can help! Check out our Instagram @springforwardpt for starting exercises for shoulder pain. And of course, Spring Forward Physical Therapy can help you! You can call our clinic at 212-996-9700 or email questions to me at anna@springforwardpt.com
REFERENCES
1. https://pubmed.ncbi.nlm.nih.gov/18411219/
2. https://pubmed.ncbi.nlm.nih.gov/10952865/
3. https://www.bmj.com/content/313/7057/601
4. https://pubmed.ncbi.nlm.nih.gov/15769790/
5. https://pubmed.ncbi.nlm.nih.gov/25184132/
6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5942400/
7. https://pubmed.ncbi.nlm.nih.gov/24847788/
8. https://www.tandfonline.com/doi/abs/10.1179/1743288X11Y.0000000027
9. https://pubmed.ncbi.nlm.nih.gov/20710088/
10. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3191586/